Really, are palliatives a major cost to the system?
Really, are palliatives a major cost to the system? Why Spain has a deficit in palliative care
Why Spain has a deficit in palliative careThe Covid-19 pandemic and its variants have forced us to take a fresh look at death and all that surrounds it. A reflection is needed to draw positive consequences from the experience. And in addition to health institutions, professionals, nurses and caregivers, academic experts are already doing so.
For example, the physician and priest Pablo Requenaa Vatican delegate to the World Medical Association, member of the Ethics Committee of the Bambino Gesú Pediatric Hospital in Rome, and professor at the University of the Holy Cross in Rome, has just written a 140-page book titled The good deathwith the suggestive subtitle Human dignity, palliative care and euthanasia.
The book will be reviewed in the October issue of Omnes magazine, but we can already glean some ideas that serve the purpose of these lines. Pablo Requena says: "In many of the current debates, euthanasia and palliative care are pitted against each other. Is this confrontation appropriate, and could euthanasia or assisted suicide not be considered a last instrument in the arsenal of palliative care? The following pages attempt to explain why the answer to this last question is in the negative. Euthanasia should not be part of medicine because it goes against its purpose, its methods and its practice".
Palliative care is notoriously supported by the Holy See, being considered as a comprehensive care of patients with intense suffering in a serious illness, in an interdisciplinary way, in order to maintain their well-being and quality of life. This was reflected in the White Book for Global Palliative Care Advocacy, White Paper in which experts from all over the world, convened by the Pontifical Academy of Life, and coordinated by the Atlantes research team of the Institute for Culture and Society (ICS) of the University of Navarra, studied formulas to promote palliative care.
Requena refers in the book to pioneers of palliative care, such as Jeanne Garnier, a young woman from Lyon who in 1835 lost her husband and two small children, and who, on the verge of despair, her strong anchoring in faith helped her to move forward, to the point of starting a welfare work for the dying abandoned by society. Thus was born the Association of the Ladies of Calvary (1842).
The author also mentions Rose Hawthorne Lathtrop, Florence Nightingale, and of course Elisabeth Kübler Ross, "a Swiss physician who did much of her work in the United States, and who is best known for her book On death and the dying (1969), in which he recounts the experience of many years and thousands of hours spent at the bedside of the sick, many of them dying".
Pablo Requena also mentions arguments of Dr. Marcos Gómez, who has dedicated his long professional life to palliative careThe company, which presented at the end of July, together with the President of the Spanish Medical Council, Dr. Tomás Cobo Castro, a Palliative Sedation Guide 2021The event was held at the Consejo General de Colegios Oficiales de Médicos (General Council of Medical Associations), prepared together with the Spanish Society of Palliative Care (Secpal).
The book also stresses, in case there was any doubt, that "The World Health Organization explains that 'palliative care improves the quality of life for patients and families coping with life-threatening illness by mitigating pain and other symptoms, and by providing spiritual and psychological support from the time of diagnosis to the end of life and during bereavement' (WHO 2020)."
In Europe, in America...
Pablo Requena's reflections and arguments help to contextualize the growing demand for palliative care, and Secpal's analysis. Europa tThe number of patients to be cared for by 2030 will be almost 5 million. with severe suffering and serious illness, compared to the current 4.4 million, while 65 % of the population still does not have access to palliative care. Thirty-eight percent will have oncological diseases, cancer; 33 percent, cardiovascular; 16 percent, variants of dementias; 6 percent, chronic; and 7 percent, others.
In Latin America, seventeen Spanish- and Portuguese-speaking countries, with 630 million people, have 1,562 palliative care teams, a ratio of 2.6 per million inhabitants. Progress is being made, but not enough, because it is estimated that only 7.6 % of people in need of palliative care in Latin America receive it, although there are already five countries (Colombia, Costa Rica, Chile, Mexico and Peru) that have a palliative care law, which Spain, for example, does not have.
Regarding the Covid-19 pandemic, data are provided for the Americas, because the American continent, out of a world total of 225.2 million infections, leads the number of confirmed cases (86.6 million), ahead of Europe (65.4 million) and Asia (64.8 million). In addition, out of a total of 4.6 million deaths up to September 12, America exceeds 2.1 million, Europe 1.2 million, Asia 1 million, Africa 202,911, and Oceania 2,582.
By country, the United States leads the list of deaths (674,639), followed by Brazil (589,277), India (442,238), Mexico (266,150), Peru (198,621), etc. Spain officially recorded 85,237 deaths on that date. In summary, of the five countries with the most deaths, four are American.
Need for specialized care
With these data, it seems logical that some organizations and institutions have begun to draw some preliminary conclusions, even lessons, learned from the Covid-19 pandemic, with implications for the treatment of patients in the face of future pandemics, and what remains of this one and its variants. Two of the most painful issues on which the experts have focused are specialized care to alleviate intense suffering, and the loneliness of the sick.
Some conclusions formulated by the Spanish Society of Palliative Care, chaired by Dr. Juan Pablo Leiva, at the 71st Meeting of the European Regional Committee of the World Health Organization (WHO), which took place from September 13 to 15, are the following:
1) "The needs for palliative care in Europe are increasing rapidly," and the health crisis "has made the imperative for its integration into health systems more urgent than ever."
2) "Pandemic preparedness should include the provision of integrated palliative care services for both those affected and non-Covid patients, including the chronically ill elderly."
3) "Basic palliative care focused from Primary Care can alleviate a significant symptom burden," but the system "needs resources."
On the other hand, Secpal demands that "all health professionals be trained to respond to patients with palliative care needs. This education should be at both undergraduate and postgraduate level. Currently, only 9 out of 51 European countries have palliative care as a compulsory subject in medical schools, and just over half of the countries provide official accreditation. Spain is one of these countries in which the lack of official accreditation in palliative care The lack of access to this care increases the barriers to access to care.
The society of palliative physicians also calls for "all essential controlled medications for symptom management, including pain and psychological distress, in particular, opioid analgesics to relieve pain and shortness of breath and benzodiazepines for sedation (Covid) to be available, accessible and affordable."
Palliative specialists denounce that "some European countries have experienced shortages and stock-outs of controlled drugs (opioids and benzodiazepines) used in Covid and palliative care." In prepandemia, for example, "25 % of European countries reported that immediate-release oral morphine was not available, and some countries have no oral morphine at all. Kazakhstan has reported having only injectable morphine and fentanyl."
Training and preparation
The training of healthcare professionals is one of the most important aspects. In this regard, Secpal points out that "thirteen European countries have recognized the specialty of Palliative Care, while in Spain there is no specific formal training to ensure that patients and their families will be cared for by the most qualified professionals to respond "to the changing, critical and complex situations generated by the process of advanced disease or end of life".
It also adds that "the Spanish Society of Palliative Care defends that the Specific Training Area (ACE) and the Advanced Accreditation Diploma (DAA) are "compatible, complementary and necessary" formulas to create an effective care structure that ensures the population "the best possible quality of life until the end"..
"One of the structural reasons for this precariousness in access to palliative care in Spain, although not the only one, is the lack of recognition of a specialty or super-specialty in the field of knowledge of palliative care, which is the most characteristic of the palliative care field. care and should meet the needs of the patient wherever he or she is, whether at home, in a hospital or in a residential center," explains Dr. Juan Pablo Leiva, president of Secpal. He therefore argues that "the ability to offer a structured response to human suffering related to the dying process "should be present at all levels of healthcare: primary and hospital care and emergency services."
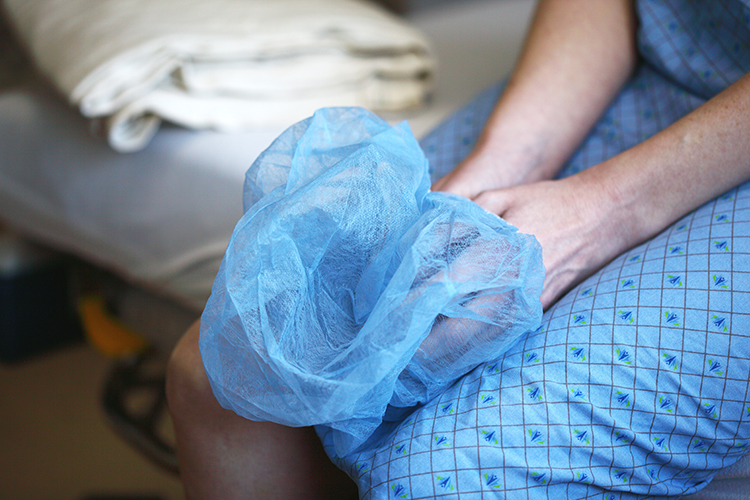
The pain of loneliness
Another objective of palliative care is to try to alleviate the loneliness of the sick, to accompany them. With regard to the provision of this care during the pandemic, Secpal provides how attempts were made to ensure care in the worst moments of the pandemic.
The same organization and the Spanish Association of Palliative Care Nurses (Aecpal), issued in unison a press release in which they demanded that people be accompanied so that they would not die alone.
As an approximation to what happened during the pandemic, the Aecpal Research Group has published in the journal Palliative Medicine a study which, based on the experience of 335 nursing professionals from all over the country, shows that 49.8 % of Covid 19 patients in the last days of life that they attended during the months of April and May were unable to say goodbye to their loved ones. Only in 6.8 % of cases did this farewell take place at the time of death.
These and other data show, according to the same sources, that, despite the existence of accompaniment protocols and the great effort made by healthcare professionals to humanize care, even to the point of giving their lives, "loneliness has been very present in patients in the last days of life, which entails a significant emotional cost for the bereaved families, as well as for the professionals themselves".
And they add that "this reality continues to occur, has increased to unbearable limits the suffering of patients and their loved ones, and can in no case be considered as dying with dignity".